Anthrax -PA Based Vaccines
Cell-free vaccines are considered safe and effective. The tripartite toxins of Bacillus anthracis are essential for the development of Anthrax, therefore can serve as excellent candidates for a protein vaccine. The toxins are composed of two enzymes, Lethal Factor (LF) and Edema Factor (EF), and a transport system composed of 7 subunits of the Protective Antigen (PA) protein. We demonstrated that a vaccine based on the PA protein, efficiently protects animal models from the deadly infection of B. anthracis spores. This vaccine is efficient in preventing infection either as a pre-infection vaccination or in combination with the antibiotic treatment, to prevent relapse of the disease. Although this vaccine is effective, we are constantly looking for additional proteins that can be added to the vaccine to improve its potency.
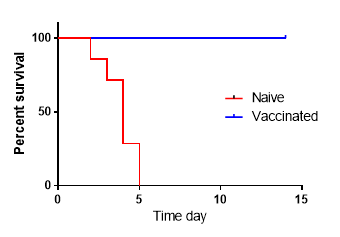
Survival of PA vaccinated or naïve animal model infected with B. anthracis spores
Mechanisms of rapid F1-mediated protective immunity against plague
Plague, initiated by Y. pestis infection, is a fatal disease that progresses rapidly and leads to high mortality rates if not treated. Antibiotics are effectively used for plague therapy, however, antibiotic-resistant Y. pestis strains have been reported and therefore alternative countermeasures are needed. In the present study we assessed the potential of an F1 and LcrV-based vaccine to provide protection shortly pre- or post-exposure to a lethal Y. pestis infection.
In this project, we have vaccinated mice up to one day before or even several hours after challenge, and found that they were effectively protected. Protection was observed despite the observation that anti-F1 and anti-LcrV titers of mice immunized one or three days pre-challenge, were below detection levels. Yet, by using B-cell deficient µMT mice we showed that rapidly-induced protective immunity requires the integrity of the humoral immune system. Analysis of the individual contribution of vaccine components to protection revealed that rF1 is responsible for the observed rapid antibody-mediated immunity. Applying anti-F1 passive therapy in the mouse model of bubonic plague demonstrated that anti-F1 F(ab’)2 can delay mortality, but cannot provide long-lasting protection as opposed to intact anti-F1 molecules. Fc-dependent immune components such as the complement system and, to lesser extent, neutrophils, contribute to mice survival. These data extend our understanding of the immune mechanisms required for development of a rapid and effective post exposure therapy against plague.
